
What is Atrial Septal Defect (ASD)?
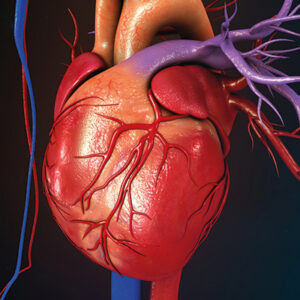
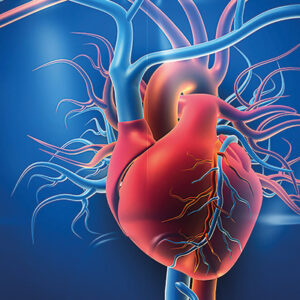
The heart normally has two upper chambers called atria and two lower chambers called ventricles. The right and left atria are separated by a wall known as the atrial septum. If a defect occurs in the formation of this wall during heart development, an opening forms between the atria. This condition is called atrial septal defect (ASD).
More than 80% of ASD cases are classified as secundum type ASD, located in the region called the fossa ovalis. This is the type suitable for non-surgical device closure. Other types are less common and are often associated with additional vascular or valve abnormalities. These types usually require surgical treatment.
In ASD, oxygen-rich blood from the left atrium passes through the opening into the right atrium and mixes with oxygen-poor blood. The amount of blood that passes depends on the size of the defect. A larger defect results in greater mixing and increased workload on the lungs and right side of the heart.
If left untreated, a large ASD may lead to enlargement of the right heart chambers, right heart failure, pulmonary hypertension, reversal of blood flow, cyanosis, paradoxical embolism, serious rhythm disorders, and even death. Early diagnosis and treatment greatly reduce these risks.
What symptoms occur in ASD patients?
Symptoms depend on the size and location of the defect and the presence of other abnormalities. Many patients, especially those with small or moderate defects, may have no symptoms. ASD is often detected incidentally during cardiac evaluation. Some patients may experience fatigue, shortness of breath, or palpitations. In advanced untreated cases, severe shortness of breath, arrhythmia, swelling in the legs or abdomen, and bluish discoloration of the lips and nails may occur.
How is ASD diagnosed?
Clinical symptoms, physical examination, and electrocardiography findings may raise suspicion. Diagnosis is confirmed with echocardiography. Most cases can be detected with transthoracic echocardiography (TTE). Transesophageal echocardiography (TEE) provides more detailed evaluation of defect size, shape, and suitability for device closure.
How is ASD treated?
There are two treatment options: surgical closure with open-heart surgery and transcatheter device closure without open surgery. Very small defects (less than 10 mm) with low shunt ratio (less than 1.5) may not require closure and can be followed regularly. Larger defects with significant shunting should be closed.
Most secundum type ASDs are suitable for device closure. Suitability is determined by TEE evaluation. If not suitable, or in other ASD types, surgical closure is performed.
How is ASD closed with a device?
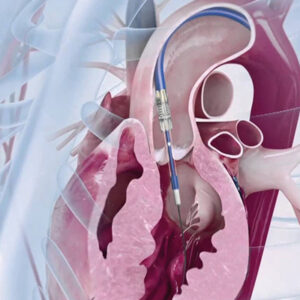
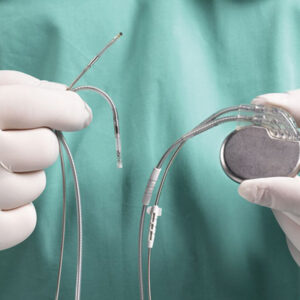
Device closure is performed in a catheterization laboratory under sterile conditions and mild sedation. Access is obtained through the femoral vein in the groin. A catheter is advanced into the right atrium and then through the defect into the left atrium. A specially designed closure device with two discs is positioned across the defect under TEE guidance. Once correct placement is confirmed, the device is released permanently, sealing the defect.
What happens if ASD is not treated?
If a significant ASD is not closed, excessive blood flow to the lungs increases pressure in the pulmonary arteries and enlarges the right heart chambers. Over time, this may cause pulmonary hypertension, right heart failure, reversal of blood flow, cyanosis, stroke due to paradoxical embolism, serious arrhythmias, and life-threatening complications. Except for very small defects with minimal shunting, timely closure is recommended.
Symptoms Of ASD In Children And Adults
Small ASDs may cause no symptoms in childhood. Larger defects can lead to frequent respiratory infections, poor weight gain, fatigue with feeding in infants, or reduced stamina in children. Some children are diagnosed after a doctor hears a heart murmur or notices signs of increased blood flow through the lungs.
In adults, symptoms often include shortness of breath with exertion, reduced exercise tolerance, palpitations, and fatigue. Some people notice swelling in the legs or episodes of arrhythmia such as atrial fibrillation or atrial flutter. Symptoms may become more noticeable with age as the right heart enlarges and pulmonary pressures rise. A small number of patients can develop stroke risk through paradoxical embolism, especially if pressures shift and right-to-left shunting occurs in advanced disease.
Potential Complications If ASD Is Not Treated
Untreated significant ASD can lead to enlargement of the right atrium and right ventricle, which may contribute to arrhythmias over time. Chronic increased blood flow to the lungs can raise pulmonary pressures, and in advanced cases pulmonary hypertension may develop. If pulmonary vascular disease becomes severe, closure may no longer be safe, which is why timing matters.
Other possible complications include right-sided heart failure, reduced exercise capacity, and stroke in specific circumstances. Many patients also develop atrial arrhythmias in adulthood, especially if the ASD is large and has been present for decades. Closing an ASD can reduce volume overload, but existing rhythm issues may still require separate treatment and monitoring.
When ASD Closure Is Recommended?
Closure is usually considered when there is evidence of a significant left-to-right shunt and right heart enlargement, even if symptoms are mild. The goal is to prevent long-term complications such as arrhythmias, heart failure, and pulmonary hypertension. Closure is also considered when symptoms are present and are likely related to the defect.
However, closure is not automatic for every ASD. If pulmonary hypertension is severe, clinicians carefully evaluate whether closure is safe. In advanced pulmonary vascular disease, closure can worsen right-sided pressures. That is why a thorough assessment of pulmonary pressures and vascular resistance is important in selected patients, particularly adults diagnosed later in life.
Catheter Based ASD Closure
Many secundum ASDs can be closed using a transcatheter device. The procedure is performed through a vein, usually in the groin. A catheter is advanced to the heart, and a closure device is positioned across the defect. The device expands on both sides of the septum to seal the opening. Over time, tissue grows over the device, creating a stable closure in most cases.
Catheter closure can offer faster recovery compared with surgery, but candidacy depends on ASD size and the presence of adequate tissue rims for anchoring. Very large defects or defects with unsuitable anatomy may not be appropriate for device closure. Patients should ask for a clear explanation of anatomy and device suitability based on detailed imaging.
Surgical ASD Repair
Surgery is recommended for primum ASDs, sinus venosus ASDs, and secundum ASDs that are too large or anatomically unsuitable for device closure. Surgical repair involves closing the defect with sutures or a patch, depending on size and location. In cases where valves are involved, surgeons may repair associated valve abnormalities during the same operation.
Surgical outcomes are generally strong in experienced centers, and repair can significantly improve long-term heart function when performed before irreversible pulmonary vascular disease develops. Recovery takes longer than catheter closure, and it typically involves a short hospital stay and a structured return to activity plan.
ASD And Arrhythmia
Atrial enlargement from long-term shunting can create a substrate for arrhythmias, especially atrial fibrillation and atrial flutter. Closing the ASD reduces volume overload, but existing electrical remodeling may not fully reverse, particularly in older adults. This is why some patients need separate rhythm management strategies even after successful closure.
Rhythm management can include medication, cardioversion, catheter ablation, and stroke prevention planning when indicated. A comprehensive care plan addresses both the structural heart issue and the rhythm issue rather than treating them as separate problems.
Living With ASD After Treatment
Many people live full, active lives after ASD closure. Activity recommendations depend on the type of repair, heart function, pulmonary pressures, and rhythm status. Some patients benefit from cardiac rehabilitation or guided exercise plans, especially if they were deconditioned before treatment.
Long-term heart health also benefits from controlling blood pressure, cholesterol, and lifestyle risk factors. While ASD is congenital, overall cardiovascular risk still matters, especially as people age. A structured follow-up plan helps ensure that any late issues, such as arrhythmias or residual shunts, are detected early.
Patent Foramen Ovale (PFO)
What is Patent Foramen Ovale (PFO)?
Patent foramen ovale (PFO) is a small opening in the thin area of the atrial septum called the fossa ovalis, which normally closes shortly after birth. If this structure does not fully close, a small flap-like opening remains between the right and left atria of the heart.
What causes PFO?
During fetal development, there is a natural opening between the right and left atria that allows blood to pass from the right atrium to the left atrium. After birth, this opening is expected to close. However, in about 25% of individuals, the closure is incomplete, leaving a small flap-like passage. As a result, PFO is present in approximately one out of every four people.
What symptoms are seen in PFO?
In most cases, PFO does not cause symptoms. Rarely, it may be associated with treatment-resistant migraine attacks or stroke. Because PFO is common in the general population, it usually does not require treatment unless complications occur. Only a small percentage of patients require intervention.
In situations that increase pressure inside the chest, such as coughing, sneezing, or straining, the flap-like opening may allow blood to pass between the atria. In certain cases, small blood clots formed in the veins of the legs or abdomen can travel to the right atrium, pass through the PFO to the left atrium, and then reach the brain or other organs. This may lead to stroke or other embolic events.
When should PFO be treated?
PFO closure may be considered in cases of unexplained stroke, treatment-resistant migraine, platypnea-orthodeoxia syndrome, and decompression illness in divers. Since PFO is common, it may be detected incidentally in patients with stroke. Therefore, before deciding on closure, other possible causes of stroke must be carefully evaluated.
Certain anatomical features increase stroke risk, such as a PFO wider than 4 mm, a long tunnel-shaped PFO, atrial septal aneurysm, prominent Eustachian valve, or spontaneous right-to-left shunting at rest.
Although the exact relationship between migraine and PFO is not fully clarified, available data suggest that closure may be beneficial in selected patients with resistant migraine.
How is PFO diagnosed?
PFO can be detected by echocardiography. Transthoracic echocardiography (TTE) may raise suspicion or confirm the diagnosis. However, transesophageal echocardiography (TEE), performed using a probe placed in the esophagus, provides more accurate evaluation. TEE determines the location, size, shape, stroke risk features, and suitability for device closure.
How is PFO treated? How is it closed?
PFO closure is a minimally invasive procedure performed in a catheterization laboratory under sterile conditions and mild sedation. Access is obtained through the femoral vein in the groin. A catheter is advanced into the right atrium and then through the PFO into the left atrium.
A special closure device with two discs is delivered through a catheter under TEE guidance. One disc is opened in the left atrium, the central waist seals the opening, and the second disc is deployed on the right atrial side. Proper positioning is confirmed with specific maneuvers. Once stability and complete closure are verified, the device is released permanently in place.
Why People Look For PFO Treatment In Turkey?
Patients explore PFO evaluation and closure in Turkey for several practical reasons. Many hospitals have advanced echocardiography services, including transesophageal echocardiography, and catheterization labs capable of performing closure procedures. International patient departments may also support appointment scheduling, medical record review, translation, and travel coordination, which can simplify the process for medical travelers.
That said, the decision to close a PFO should be based on clinical evidence, not convenience. High-quality centers prioritize thorough evaluation, often involving both cardiology and neurology when stroke is part of the story. A trustworthy team will explain the level of certainty that the PFO contributed to symptoms and will discuss both procedural and non-procedural options.
Symptoms And Signs
One of the most confusing aspects of PFO is that it often causes no symptoms. Many people discover they have a PFO during tests performed for unrelated reasons. When symptoms do occur, they are usually related to associated events such as stroke or transient neurological symptoms. Some individuals report shortness of breath in specific positional situations, or a history of decompression issues during diving.
If you have had a stroke or TIA, symptoms might include sudden weakness, speech changes, vision disturbance, facial drooping, or balance problems. Those symptoms require urgent evaluation regardless of suspected PFO. A PFO diagnosis is only one part of a broader stroke investigation and should not replace a full work-up of other potential causes.
How PFO Is Diagnosed In Turkey?
PFO diagnosis typically begins with echocardiography, an ultrasound test that visualizes heart structures. A standard transthoracic echocardiogram may detect PFO in some cases, especially when a bubble study is performed. In a bubble study, saline with tiny air bubbles is injected into a vein while the heart is imaged. If bubbles appear in the left atrium shortly after entering the right atrium, it suggests a right-to-left shunt.
Transesophageal echocardiography often provides a clearer view of the atrial septum and can help assess PFO features, including tunnel length and associated septal aneurysm. Some centers may use transcranial Doppler as an additional method to detect shunting. For patients evaluated after stroke, the diagnostic pathway usually includes brain imaging, vascular imaging, rhythm monitoring for atrial fibrillation, blood tests, and risk factor assessment.
How Doctors Decide If PFO Closure Is Appropriate?
The decision to close a PFO is based on overall clinical context. In patients with cryptogenic stroke, clinicians evaluate whether the stroke could have been caused by other mechanisms, such as atrial fibrillation, carotid disease, small vessel disease, or clotting disorders. If no other cause is found and the patient profile fits evidence-based criteria, PFO closure may be considered.
Factors that may influence the decision include age, stroke type and imaging features, presence of a large shunt, associated atrial septal aneurysm, and overall vascular risk. A careful discussion should include the benefits, risks, and alternatives such as antiplatelet therapy or anticoagulation when indicated. Good decision-making is personalized and aims to reduce future stroke risk without adding unnecessary procedural risk.
PFO Closure In Turkey
PFO closure is usually a transcatheter procedure performed in a catheterization laboratory. A thin catheter is inserted through a vein, often in the groin, and guided to the heart. The closure device is delivered to the atrial septum and deployed to seal the opening. The device typically has two discs that sit on either side of the septum and stabilize in place. Over time, heart tissue grows over the device, creating a permanent seal in most cases.
The procedure is often performed under sedation or general anesthesia depending on hospital protocol and imaging requirements. Intraprocedural imaging helps confirm correct positioning. Patients are monitored afterward and may stay in the hospital for observation. Discharge planning includes medication instructions and follow-up imaging to confirm closure success and detect rare complications.
































I would like to express my sincere thanks and appreciation to Prof. Dr. Hasan Turhan and the entire medical team who performed my EPS ablation procedure. 🙏🏻
Prof. Dr. Hasan Turhan is one of the leading physicians in his field. He had been closely following my mother’s condition for a long time. When surgery became necessary for her full recovery, the procedure was performed successfully.After the operation, my mother experienced pain, and he stayed by her side from midnight until 4:00 a.m. without leaving even for a moment. I told him personally that even a close relative could not have shown more care.We are deeply grateful for his patience, precision, and the way he explains everything clearly and simply. He answered all our questions in a direct and understandable manner.Our sincere thanks to Prof. Dr. Hasan Turhan, and especially to Ms. Hamide, Ms. Fatma, and all the doctors, nurses, and healthcare staff in the service.
We visited Prof. Dr. Hasan Turhan due to my spouse’s heart rhythm disorder. Although other hospitals recommended ablation, we were afraid and postponed the procedure. We spent weeks in different emergency departments across Istanbul.Meeting Prof. Dr. Hasan Turhan was truly a turning point for us. He is highly experienced, confident, and reassuring in his field. At first, we hesitated again and preferred to try medication. However, we eventually underwent the ablation procedure.After the treatment, we realized we should have done it much earlier. The procedure was very successful, and we returned to our normal life. If you have any heart-related concerns, Prof. Dr. Hasan Turhan is truly an expert in his field.Thank you for everything.
Prof. Dr. Hasan Turhan is a rare physician distinguished by his medical expertise, professional discipline, and strong human values.When I consulted him for my heart rhythm disorder, the knowledge, skill, and mastery he demonstrated during my treatment were truly beyond words.I am sincerely grateful to my esteemed colleague, thanks to whom I have regained my health. Wishing him continued success and good health.Dr. Numan Bakırcı