
What is peripheral artery disease (PAD)?
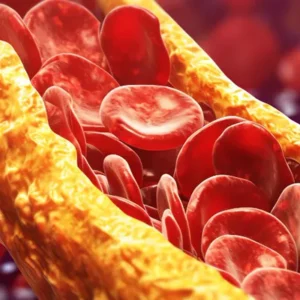
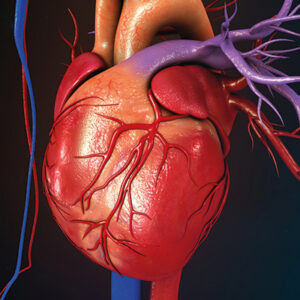
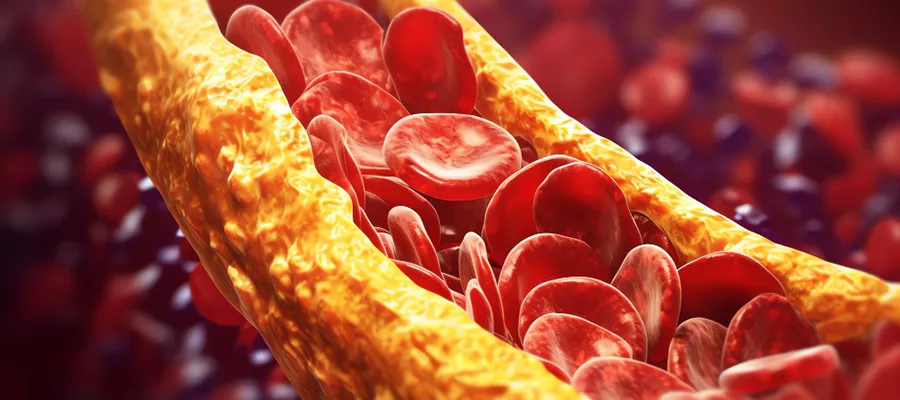
Peripheral artery disease is a circulatory disorder caused by narrowing or blockage of the arteries that carry blood to the arms and legs. Similar to coronary artery disease, it usually begins with the formation of atherosclerotic plaques, which involve fat accumulation and calcification in the vessel wall. Over time, these plaques lead to significant narrowing or blockage, reducing blood flow to the tissues. As a result, a condition called ischemia, meaning inadequate blood supply to the tissue, develops.
What are the risk factors for peripheral artery disease?
Risk factors for vascular disease are generally similar throughout the body. The same risk factors apply to coronary artery disease, carotid artery disease, and arm or leg artery disease. These include smoking, hypertension, hyperlipidemia, diabetes, obesity, a sedentary lifestyle, stress, and advanced age. Peripheral artery disease is more common in men than in women.
What symptoms occur in peripheral artery disease?
In the early stages, when there is no severe narrowing or blockage, patients may have no symptoms. As the narrowing progresses, poor circulation develops below the affected area. During activities such as walking, climbing stairs, or running, reduced blood flow may cause pain and cramping in the calves, thighs, hips, or arms. These symptoms usually improve with rest. In advanced stages, pain may occur even at rest, and wounds or gangrene may develop in the feet or hands.
How is peripheral artery disease diagnosed?
The presence of typical symptoms and risk factors raises suspicion of peripheral artery disease. During physical examination, the absence of a pulse in one or more arteries is an important finding.
Measuring blood pressure in the arms and legs and calculating the ankle-brachial index (ABI) is a simple and reliable diagnostic test.
Doppler ultrasonography can evaluate the presence, location, and severity of narrowing.
If necessary, angiography of the leg or arm arteries may be performed.
How is peripheral artery disease treated?
Treatment includes lifestyle changes, medication, interventional procedures, and surgical options.
Lifestyle modification is essential at every stage of the disease. In early stages, it may slow progression and delay or prevent the need for intervention or surgery.
Treatment decisions depend on multiple factors, including the location and severity of the disease, its extent, the patient’s age, and accompanying medical conditions.
While surgical methods were previously common in severe and widespread disease, today minimally invasive endovascular treatments often provide better outcomes for many patients.
Interventional treatment methods for peripheral artery disease include:
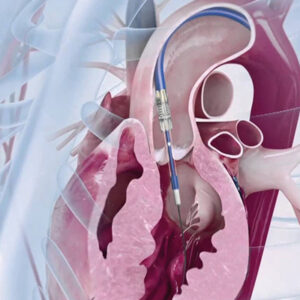
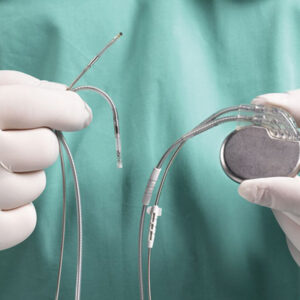
- Balloon angioplasty (PTA): A catheter with a balloon is advanced to the narrowed segment and inflated to widen the vessel. This is the most commonly preferred and effective method.
- Stent placement: A metal mesh structure inserted to keep the vessel open if balloon angioplasty alone is insufficient or to prevent re-narrowing.
- Atherectomy: Removal of plaque from inside the artery by shaving the obstructive material.
Common Symptoms Of Peripheral Artery Disease
The classic symptom of PAD is intermittent claudication, which is cramping, aching, or tightness in the calf, thigh, or buttock that appears during walking and improves with rest. The location of pain can hint at which artery segment is affected. Some patients describe heaviness, fatigue, or a burning sensation rather than sharp pain.
Other signs can include coldness in the lower leg or foot, numbness or weakness, reduced hair growth on the legs, shiny skin, slow-growing toenails, and weaker pulses in the feet. In advanced disease, patients may develop rest pain, especially at night, or ulcers on the toes or feet that heal slowly. Sudden severe pain, pale skin, or loss of sensation can signal acute limb ischemia, which requires emergency medical care.
Why PAD Is Often Missed
PAD is underdiagnosed because symptoms can be mistaken for arthritis, sciatica, or general aging. Some patients reduce activity unconsciously to avoid discomfort, which hides the pattern of pain with exertion. People with diabetes may have nerve damage that reduces pain sensation, allowing PAD to progress without typical warning signs.
Because PAD indicates systemic atherosclerosis, missing the diagnosis can mean missing an opportunity to prevent heart attack and stroke. If you have risk factors and notice exertional leg discomfort, it is worth asking for a vascular evaluation.
Stages Of PAD And What Critical Limb Ischemia Means
PAD severity ranges from mild narrowing with no symptoms to advanced disease with rest pain and ulcers. A key concept is chronic limb-threatening ischemia, sometimes called critical limb ischemia. This occurs when blood flow is so limited that tissues cannot survive without improved circulation. Patients may have non-healing wounds, gangrene, or persistent rest pain.
Chronic limb-threatening ischemia requires urgent specialist evaluation because the goal is limb salvage and prevention of infection and amputation. Treatment often involves revascularization combined with wound care, infection management when present, and aggressive risk factor control.
Lifestyle Treatment And Risk Factor Control
PAD treatment begins with cardiovascular risk reduction. Smoking cessation is essential, and stopping smoking can slow progression and improve outcomes after procedures. Diabetes control, blood pressure management, and cholesterol lowering are also central because PAD is linked to systemic plaque buildup.
Diet and exercise play major roles. Heart-healthy eating patterns that emphasize vegetables, fruits, legumes, whole grains, lean proteins, and unsaturated fats support vascular health. Weight management and regular activity improve metabolic factors and can reduce symptoms over time.
Supervised Exercise Therapy For PAD
Supervised exercise therapy is one of the most effective non-procedural treatments for intermittent claudication. It typically involves structured walking sessions where patients walk until moderate discomfort, rest, and repeat. Over time, this improves walking distance and reduces symptom impact. The mechanism includes better muscle efficiency, improved circulation through collateral pathways, and improved overall fitness.
Many patients are surprised that walking into mild discomfort can be part of therapy, but when done safely under guidance, it can significantly improve quality of life. Consistency is the key. If supervised programs are not available, a carefully designed home walking plan can still help, but supervision often improves adherence and results.
Medications Used In PAD Management
Medication treatment typically targets both symptoms and cardiovascular risk. Antiplatelet therapy is commonly recommended to reduce the risk of heart attack and stroke in many PAD patients. Statin therapy is also central because it lowers LDL cholesterol and helps stabilize plaque. Blood pressure medications and diabetes treatments are adjusted to protect blood vessels and organs.
In some patients with claudication, medications may be considered to improve walking distance, depending on regional guidelines and patient profile. The most important point is that medication is not only about symptom relief. It is about lowering systemic risk and preventing future major cardiovascular events.
Endovascular Treatment Options
When lifestyle and medication are not enough, or when symptoms severely limit life, endovascular procedures may be considered. These are minimally invasive treatments performed through small access points in the artery. Balloon angioplasty can widen a narrowed vessel, and stents may be placed to keep the artery open. In some cases, drug-coated balloons or specialized devices are used to reduce the chance of re-narrowing in certain artery segments.
Endovascular therapy can offer shorter recovery times compared with open surgery, but outcomes depend on lesion length, location, vessel size, and patient factors such as diabetes and smoking. A vascular specialist will consider both symptom relief and durability when recommending an approach.
Surgical Treatment Options For PAD
Surgery may be recommended when blockages are extensive, when endovascular therapy is unlikely to be durable, or when chronic limb-threatening ischemia requires robust revascularization. Common surgical approaches include bypass surgery, where blood flow is rerouted around the blockage using a graft vessel. Endarterectomy, which removes plaque from the artery, may also be used in selected locations.
Surgical treatment can be highly effective, but it involves a larger procedure and longer recovery. Preoperative risk assessment is important because PAD patients often have coexisting coronary artery disease or other conditions. The best outcomes come from a strategy that balances procedural risk with long-term benefit.
Wound Care And Limb Protection In Advanced PAD?
For patients with foot ulcers or tissue loss, wound care is an essential part of treatment. Revascularization alone may not be enough if infection is present or if wound care is inconsistent. Specialized wound management, pressure offloading, appropriate footwear, and diabetes management can dramatically influence healing.
Patients should examine their feet regularly, especially if they have diabetes or neuropathy. Early attention to minor injuries prevents progression to serious infections. Any non-healing wound, especially on toes or the sole, should trigger prompt vascular evaluation.































I would like to express my sincere thanks and appreciation to Prof. Dr. Hasan Turhan and the entire medical team who performed my EPS ablation procedure. 🙏🏻
Prof. Dr. Hasan Turhan is one of the leading physicians in his field. He had been closely following my mother’s condition for a long time. When surgery became necessary for her full recovery, the procedure was performed successfully.After the operation, my mother experienced pain, and he stayed by her side from midnight until 4:00 a.m. without leaving even for a moment. I told him personally that even a close relative could not have shown more care.We are deeply grateful for his patience, precision, and the way he explains everything clearly and simply. He answered all our questions in a direct and understandable manner.Our sincere thanks to Prof. Dr. Hasan Turhan, and especially to Ms. Hamide, Ms. Fatma, and all the doctors, nurses, and healthcare staff in the service.
We visited Prof. Dr. Hasan Turhan due to my spouse’s heart rhythm disorder. Although other hospitals recommended ablation, we were afraid and postponed the procedure. We spent weeks in different emergency departments across Istanbul.Meeting Prof. Dr. Hasan Turhan was truly a turning point for us. He is highly experienced, confident, and reassuring in his field. At first, we hesitated again and preferred to try medication. However, we eventually underwent the ablation procedure.After the treatment, we realized we should have done it much earlier. The procedure was very successful, and we returned to our normal life. If you have any heart-related concerns, Prof. Dr. Hasan Turhan is truly an expert in his field.Thank you for everything.
Prof. Dr. Hasan Turhan is a rare physician distinguished by his medical expertise, professional discipline, and strong human values.When I consulted him for my heart rhythm disorder, the knowledge, skill, and mastery he demonstrated during my treatment were truly beyond words.I am sincerely grateful to my esteemed colleague, thanks to whom I have regained my health. Wishing him continued success and good health.Dr. Numan Bakırcı